Top Tips for Making Ultrasound-Guided Vascular Access Procedures More Efficient

The utilization of ultrasound with aiding in vascular access procedures has been a regular practice for nearly four decades. Over that time, a great deal has been learned about the best ways to optimize the efficiency of ultrasound within such procedures, ensuring that patients receive the best, most streamlined care possible. Of course, knowing which ideas to implement - and how and when to implement them - can be challenging.
At CIVCO, we understand that you're busy, which is why we've gone ahead and done most of the digging for you. Compiled below are 5 surefire tips for ways to expedite your workflow and make your ultrasound-guided vascular access procedures even more efficient.
Let's dive in.

Tip #1: Choose the right transducer:
Ultrasound transducers come in a variety of different shapes and sizes...but choosing the right transducer for the right procedure is an important step when preparing how you plan to approach an upcoming scan, especially when you are trying to save time. Two of the more commonly used types of transducers are 'linear probes' and 'curvilinear probes.' There are a few key things to recognize about both types of transducers before utilizing them:
Linear probes:
- Features a rectangular beam.
- Usually reserved for superficial anatomy, due to their higher frequency, which allows for greater degrees of detail and resolution in the image.
- Not able to penetrate as deeply into the body as other probes.
Curvilinear probes:
- Features curved array that allows for a wider field of view.
- Usually reserved for abdominal sonography or technically difficult patients.
- Possesses a lower frequency that sends the beam deeper into the body, allowing for more in-depth examinations.
- Usually feature a higher color sensitivity, in order to allow physicians to find a deep vessel and identify it with the color.
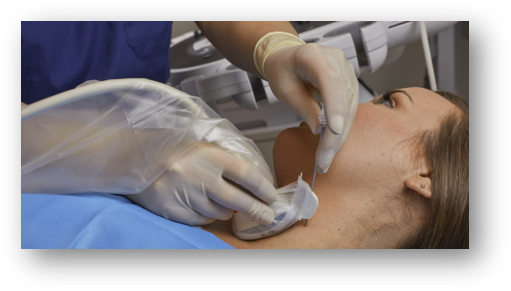
Tip #2: Choose the right needle placement technique:
When it comes to performing needle placement procedures, sonographers have a choice between performing the procedure either "free-hand" or "mechanically." Both offer distinct advantages and disadvantages, with the efficiency of each technique depending greatly on the experience and skill set of the individual user:
Free-hand technique:
Advantages
- Ideal for superficial vessels like IJV and SCV.
- Works well, provided that the ultrasound beam is not more than 90 degrees to the target.
Disadvantages:
- Challenging to access deep and hard-to-reach vessels.
- Potentially longer procedure time.
- Poor needle tip visualization can lead to unsuccessful outcomes or unwanted adverse effects.
Mechanical needle guide technique:
Advantages:
- Allows pre-planning (targeting).
- The variable angle provides flexible needle entry.
- Keeps the needle in-plane for continuous needle shaft and tip visualization.
- In-plane and out-of-plane capabilities.
- Quick release.
Disadvantages:
- Limited angle entry.
- A custom bracket is required for each probe.
- Increases the probe bulkiness.
- Retention of the non-disposables.
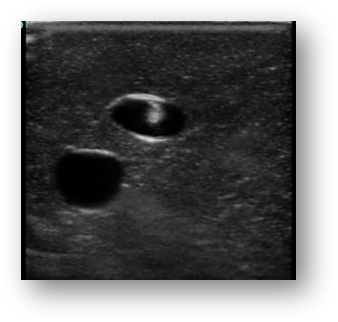
Tip #3: Choose the right needle guidance technique:
Also important is choosing the optimal needle guidance technique for your procedure. While both in-plane needle and out-of-plane needle guidance techniques can be utilized, it's important to understand exactly what each technique brings to your vascular access procedure...as well as some of the distinct challenges that are inherent to both approaches. Here is a breakdown of what makes each technique helpful AND challenging.
In-plane needle guidance:
How is in-plane needle guidance helpful?:
- The needle tip and shaft are visualized during the entire procedure.
- Some guides do not use pre-determined angles, allowing for entry angles to be adjusted continuously while keeping the needle in line with the beam.
- Can be performed freehand or with the assistance of a needle guide.
How is in-plane needle guidance challenging?:
- Visibility of the needle is primarily dependent on the angle of the needle with the transducer face, with a larger angle rendering the needleless conspicuous.
- Some guides do have predetermined angles, while also requiring accompanying software on the ultrasound machine.
- No guidelines are displayed on the screen.
Out-of-plane needle guidance:
How is out-of-plane needle guidance helpful?:
- Allows the user to align the needle to pass through a predetermined depth.
- quick release function.
- Typically performed using a free-hand technique.
How is out-of-plane needle guidance challenging?:
- Generally provides less consistent needle visualization when compared to the in-plane approach.
- The portion of the needle that intersects the sound beam is quite small.
- The needles themselves are often very small (18-25 gauge).
- Identifying the tip can be challenging.

Tip #4: Make sure you follow compliance guidelines:
Maintaining proper compliance with your probe disinfection processes isn't just important - it's highly recommended. According to AIUM 1, "Additional care needs to be taken for infection control while using ultrasound equipment to aid in procedural guidance, particularly in central vascular access, where sterility must be maintained."
Adherence to infection control guidelines is also imperative if you want to continue to ensure streamlined, complication-free vascular access procedures. AIUM recommends integrating the following recommendations to help maintain compliance:
- "Sterile probe covers should be readily available with all equipment."
- "An additional person is often required to assist with sterile preparation of the ultrasound probe and machine operation."
- "Consistent adherence to additional infection control guidelines, including hand hygiene, the use of chlorhexidine skin preparation, and maximum sterile barrier precautions, has been shown to contribute significantly to positive patient outcomes in central vascular access."
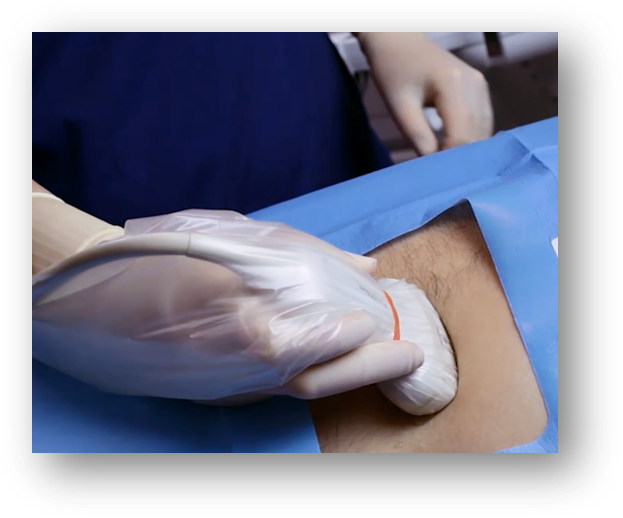
Tip #5: Choose the right probe cover:
Making sure that you choose the right probe cover is a surefire way to ensure that your vascular access procedure remains as efficient as possible...but choosing the wrong probe cover can cost you and your patient, potentially even more than just time. There are several criteria to consider when choosing a probe cover, including:
- The quality and type of material, specifically in regards to ease-of-use, patient comfort, latex vs. non-latex, etc.
- The configuration of the cover on the probe, i.e. size, length, width.
- How easy it is to deploy and remove the cover from the probe.
- Whether the probe cover has been FDA cleared and validated as a viral barrier for an ultrasound. Steer clear of condoms and bandages, such as Tegaderm and Opsite, as none are FDA-cleared for use as ultrasound probe covers, and in fact, may even have the potential to either damage the probe or leave residue behind that could harbor bacteria.
- Determine if ultrasound gel is necessary for the procedure or examination. Consider utilizing either gel-free viral barriers or Envision probe covers and scanning pads, which allow you to cover the ultrasound probe and scan without ever having to use ultrasound gel. Envision reduces the risk of contamination during CVC or PICC line placements, scanning, intraoperative procedures, and other interventions, while also streamlining your workflow by removing the need to clean up after messy ultrasound gel.
Raise Your Hand if You're Frustrated by Ultrasound Gel
As the use of ultrasound increases, so have reports of infections traced back to ultrasound gel (did you hear about the MASSIVE gel recall?).
If you're one of the many clinicians who is fed up with the infection risk and mess of gel, we have good news: You can go 100% gel-free.
Envision Ultrasound Covers and Pads are activated by sterile saline and can reduce the risk of infection while eliminating the need for gel at the insertion site.
The future of ultrasound is gel-free.
Try it for free by: REQUESTING A SAMPLE
References:
- 2012, The Association for Medical Ultrasound. "AIUM Practice Guidelines for the Use of Ultrasound to Guide Vascular Access Procedures."





